Dear Editor,
I had worked at GPHC for over 10 days seeing this patient’s husband looking very sad in the ward; his wife was diagnosed with obstructive jaundice. A CT scan was done and there was a tumour at the head of the pancreas. She was waiting for surgery for almost 10 days. During these days she felt more pain and the jaundice became more severe due to bad medical conditions in Guyana. I arranged a team to come to GPHC because it is the best hospital in Guyana, however if my team is on call the same day as we are operating, emergency cases take precedence over the patients for elective surgery and these are delayed and pushed back to another date.
I researched this case and found that it was very complicated due to the location of the tumour and that it had invaded the common bile duct and mesenteric vein, her jaundice was worsening and protein levels were low. Her pain was so severe we could not sufficiently treat it with only medication. Due to the lack of resources, such as MRI, contrast CT, albumin and plasma we were unable to assess the patient pre-operatively and post-operatively unable to give sufficient nutrients to aid in the duration of treatment. I did not want to operate due to the high risk however because of the patient’s pain and her family’s hopefulness in the doctors we proceeded.
The night before the operation my team and I planned and read articles in preparation for surgery. We discussed all the possible outcomes that could happen during the operation. I even got advice from my teacher back in China.
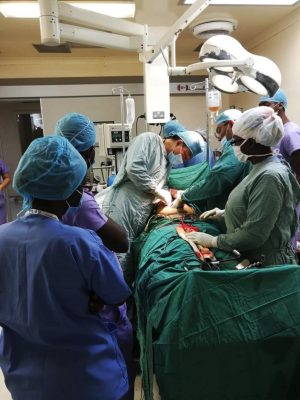
On July 19, 2018 we began the operation, we found that the situation was much worse than anticipated. The tumour was bigger and invaded the common bile duct, the mesenteric vein, multiple lymph nodes were present and organs were edematous; the liver had changed colour due to over storage of bile. The decision was made to put in T-tube drainage and block the abdominal nerve with 95% pure alcohol which has never been done in this hospital. It is dangerous to block this nerve because of its location. It is located next to the inferior vena cava and close to the aorta which is the biggest vein and artery respectively. Also, if the alcohol went into the patient’s blood stream she could have died immediately. Before injecting the alcohol anaesthesia special attention was paid to the patient’s vital signs. We located the correct point for injection of the alcohol and proceeded. At first there was a complication with the injection, the nerve was then compressed and position readjusted. I advised anaesthesia once more and at last the operation was finished.
The next morning even though it was only one day post-op the patient told us she was feeling much better and we knew the surgery was a success and all the doctors said that the outcome was “amazing!”. My colleague, Dr. Motilall, told us that there are many patients like this and this operation would be very useful for these patients. They have never done any operation like this before in Guyana.
Even though I was smiling at the time, I regretted in my heart that we could only relieve her symptoms and not cure her. The only thing we can do is to relieve her pain and help her live the rest of her life with respect. If these patients came to hospital earlier and the medical condition was much better so that we can assess the patient’s situation correctly; we would have a chance to resect the tumour completely and after operation the patients can receive sufficient nutrition to sustain their life. It was perfect and the smiling of the patient and her family will be with me forever. That’s all we want as a doctor.
Yours faithfully,
Zhang Biao
Chinese Medical Team