The Maternal and Child Health Unit of the Ministry of Public Health is seeking to expand its available family-planning options with the introduction of new, long-acting reversible contraceptive for women.
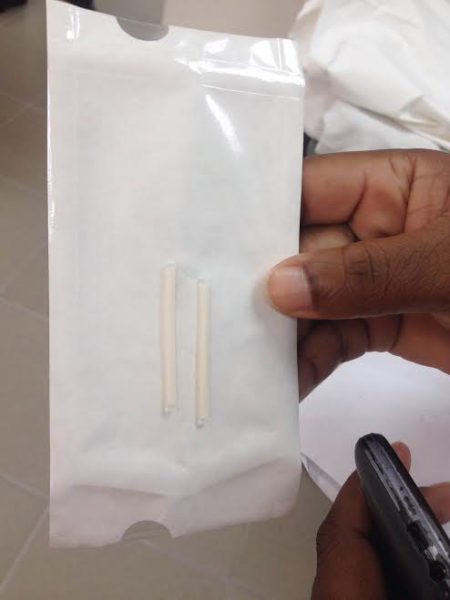
The ‘implant’ Jadelle (levonorgestrel), comes in two Progestin-filled tiny, reversible rods, the size of which can be compared to a matchstick. As the name implies, the rods are inserted just under the skin of a woman’s arm by a certified health care provider under aseptic conditions.
Once inserted, this form of contraceptive provides highly effective protection against pregnancy for up to five years and boasts an average pregnancy rate of less than 1%.
As part of the plans to integrate this new contraceptive into its available family planning services, the Maternal and Child Health Unit of the Ministry of Public Health made the implant available yesterday at the new Maternity Wing of the Georgetown Public Hospital to interested women.
Director of the Maternal and Child Health Unit Dr Ertenisa Hamilton, who was there to receive the implant herself, told Stabroek News that the ministry’s decision to add a new contraceptive to its list of available options, came as a result of wanting women to have more options.
“One of the things about family planning is that the choice must be the woman’s, which means she shouldn’t make a choice because these are the only options offered by the system. The more options they have, the more you have available, the more effective you are in meeting the need of the actual patient, customer, consumer who comes for family planning services,” Hamilton added.
She stated that while the implant is long acting, it is also reversible, meaning the rod can be removed upon request, allowing the woman to conceive as normal, if so desired.
“If you are young and not ready for a family you can have it, just as if you have children and are not ready for more…,” she added.
Additionally, she said women would be offered counselling before receiving family planning, in accordance with the ministry’s regulations, where possible side effects will be discussed as well as resolutions of same.
Important to note, however, is the fact that the contraceptive does not protect against sexually transmitted infections.
Meanwhile, Dr Mark Hathaway, an Obstetrician and Technical Advisor for Family Planning and Reproductive Health at Unity Health Care Inc in Washington and Senior Technical Advisor for Reproductive Health of Jhpiego, an international non-profit health organization affiliated with Johns Hopkins University, described the contraceptive as being the “one of the safest, simplest and effective methods” that is used internationally by women.
He explained that there are two type of implants. The one being used here, Jadelle, is a two-rod implant system. The other is a one rod implant which was designed by another company. He said both were similar in terms of their effectiveness and how they work.
The obstetrician explained that the primary mechanism of action of the implants include thickening cervical mucus, making it difficult for sperm to penetrate and preventing ovulation in about half of menstrual cycles.
He added that not only is the insertion of the rods painless, but they become effective almost immediately and the use of this method of family planning has been linked to a decrease in a high number of unintended pregnancies.
Commenting on the possible side effects of using this specific form of family planning, Hathaway explained the most common one to be the occurrence of irregular vaginal bleeding which is not harmful.
Additionally, Hathaway noted that unlike the propensity of the progesterone pill to cause a decrease in the bone density, the implant does not affect bone density.
“It is a historic moment at the GPHC with the first set of implants being done today,” the doctor shared, while stating that the first run at the hospital saw an average of 30 women visiting the institution to receive their implants.
Meanwhile, according to Hamilton, Hathaway’s presence at the hospital was due to him facilitating the training that was needed for the relevant members of staff. And while he is expected to depart today, the local team of health professionals will continue to work under supervision.
Later this month, however, a medical team will visit to certify the persons who would have completed the criteria according to their standards.
The Implant is being offered free of cost to interested women at the Guyana Responsible Parenthood Association (GRPA). However, Dr Hamilton said she envisions the new contraceptive becoming available in all regions within the next two years or less as part of the normal family planning services that are currently offered.
Meanwhile, the World Health Organisation has described long-acting reversible contraceptives such as implants and intrauterine devices as having have multiple advantages over other reversible methods.
Most importantly, once in place, they do not require daily or monthly dosing and their duration of contraceptive action ranges from 3 to 5 years.
Additionally, implants are registered in more than 100 countries, including the United States, Western European countries, as well as many middle and low-income nations. In 2012, the United Nations Commission on Life-Saving Commodities for Women and Children endorsed contraceptive implants as one of its 13 life-saving commodities.
The brand being used here, Jadelle, is not available for use in the United States.